Understanding Spider Veins: Causes, Risks, And Treatment Options
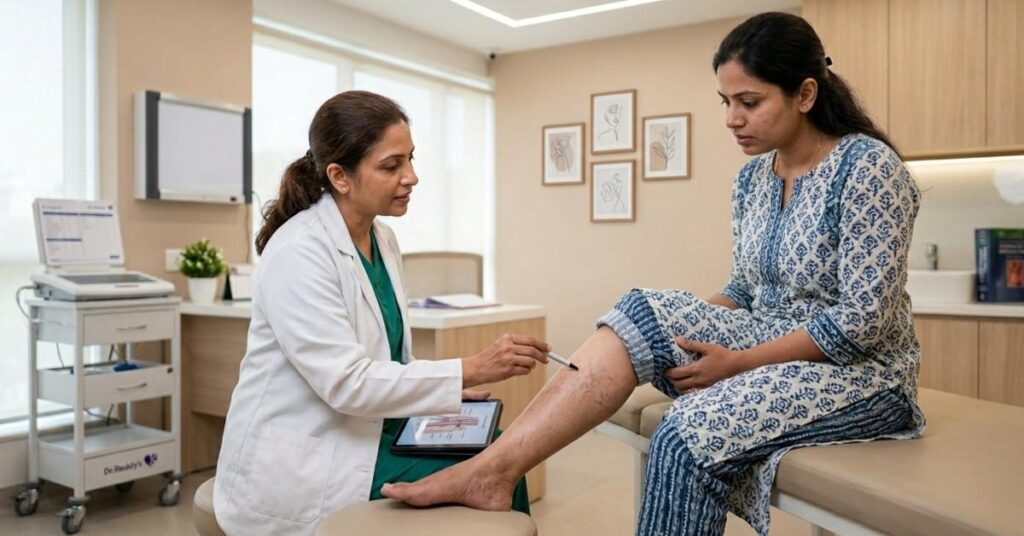
Understanding Spider Veins: Causes, Risks, And Treatment Options Understanding Spider Veins: Causes, Risks, And Treatment Options Spider veins, also known as thread veins or telangiectasia, are a common cosmetic concern characterized by clusters of small, dilated blood vessels visible near the skin’s surface. While typically harmless, they can indicate underlying venous insufficiency, where the blood flow through veins is compromised. Causes of Spider Veins: Spider veins often stem from venous insufficiency, triggered by damaged or weakened vein valves. This impairment leads to blood pooling, resulting in the formation of spider veins. Several factors contribute to their development: Genetics: A family history of spider or varicose veins increases susceptibility. Age: With aging, veins lose elasticity, making them prone to weakening. Gender: Women are more predisposed to spider veins than men. Pregnancy: Hormonal changes and increased vein pressure during pregnancy elevate the risk. Obesity: Excess weight puts additional pressure on veins, exacerbating the likelihood of spider veins. Prolonged sitting or standing: Extended periods of immobility strain veins, fostering spider vein formation. Sun exposure: Prolonged exposure to sunlight can damage skin and veins, heightening the risk. Treatment Options: Vein Ablation: This minimally invasive procedure involves inserting a catheter into the affected vein, using heat to close or shrink it. By rerouting blood flow through healthier veins, spider vein visibility decreases. Vein ablation is swift, relatively painless, and entails minimal downtime. Sclerotherapy: During sclerotherapy, a solution is injected into affected veins, causing irritation and subsequent collapse. This stops blood flow, prompting the vein to shrink and fade away. It’s effective for both spider and varicose veins and offers rapid results. Physical and Occupational Therapy: These therapies complement other treatments by improving circulation, strengthening leg muscles, and addressing lifestyle factors contributing to venous insufficiency. They can alleviate symptoms and prevent future spider veins. Understanding the causes, risk factors, and treatment options for spider veins is crucial for effective management. While they’re often a cosmetic concern, they can signify underlying venous issues that warrant attention. With a range of treatments available, including vein ablation, sclerotherapy, and therapy interventions, individuals can address spider veins and achieve healthier, more beautiful skin. If you’re concerned about spider veins, don’t hesitate to seek guidance from medical professionals for personalized assessment and treatment recommendations. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Navigating Menopause: Understanding The Transition And Treatment Options

Navigating Menopause: Understanding The Transition And Treatment Options Menopause marks the cessation of menstrual cycles, typically diagnosed after 12 consecutive months without a period. It commonly occurs in a woman’s late 40s or early 50s. This natural biological process, however, brings about various physical and emotional symptoms that can impact daily life. Symptoms and Causes: Menopause may manifest with irregular periods, vaginal dryness, hot flushes, chills, night sweats, sleep disturbances, mood changes, weight gain, thinning hair, and loss of breast fullness. Menopause results from declining reproductive hormones, particularly estrogen and progesterone, as women age. Surgical interventions such as oophorectomy or hysterectomy, cancer therapies like chemotherapy or radiation, and primary ovarian insufficiency can also induce menopause. Complications: Cardiovascular Disease: Decreased estrogen levels elevate the risk of heart and blood vessel diseases, necessitating lifestyle modifications and regular monitoring. Osteoporosis: Postmenopausal bone density loss increases the risk of fractures, emphasizing the importance of preventive measures. Urinary Incontinence: Vaginal and urethral tissue changes contribute to urinary symptoms, requiring pelvic floor exercises and possibly hormone therapy. Sexual Function: Vaginal dryness and decreased sensation may affect sexual activity, with treatments including vaginal moisturizers, lubricants, and local estrogen therapy. Weight Gain: Metabolic changes during menopause may lead to weight gain, necessitating dietary adjustments and regular exercise. Diagnosis and Treatment: Menopause is typically diagnosed based on symptoms, with blood tests to measure follicle- stimulating hormone (FSH), estrogen, and thyroid-stimulating hormone (TSH) levels in certain cases. While menopause itself requires no medical intervention, treatments focus on alleviating symptoms and managing associated conditions. Options include hormone therapy (estrogen or estrogen-progestin combinations), vaginal estrogen, low-dose antidepressants, gabapentin, and medications for osteoporosis prevention or treatment. Navigating menopause involves understanding its symptoms, causes, complications, and available treatments. With proper management and support, women can embrace this life stage with confidence and maintain their overall health and well-being. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Managing Vaginal Yeast Infections In The Heat Of Summer
Managing Vaginal Yeast Infections In The Heat Of Summer A vaginal yeast infection is a common condition affecting the vaginal area, caused by the overgrowth of a fungus called yeast. Although small amounts of yeast naturally inhabit the vagina, an imbalance leading to excessive growth can result in an infection. While yeast infections can occur anytime, certain factors, especially during warm weather, increase susceptibility. Symptoms and Diagnosis Key symptoms of a vaginal yeast infection include itching in the vaginal area, white discharge that can range from watery to thick, and redness, swelling, and burning. Pain during urination or sexual intercourse is also common. Diagnosis typically involves a medical examination where a healthcare provider checks for signs of infection and may collect a sample of vaginal fluid for lab testing. Causes and Risk Factors Yeast infections can be influenced by various factors beyond just the warm weather. Pregnancy, illnesses such as HIV or diabetes, certain medications (like antibiotics, birth control pills, and cortisone-type drugs), stress, and lack of sleep can all contribute to an increased risk. Additionally, wearing tight clothing and staying in wet swimsuits for prolonged periods can trap moisture, creating an ideal environment for yeast growth. Treatment Options Treating a vaginal yeast infection involves using antifungal medications, available in forms like pills, creams, ovules, or ointments. Treatment duration can range from 1 to 7 days, depending on the severity and the individual’s health condition. It is crucial to complete the prescribed treatment to avoid recurrent infections, particularly if underlying health issues such as diabetes are not well-managed. Prevention Tips Preventing yeast infections involves adopting several lifestyle and hygiene practices: Wear Breathable Underwear: Cotton is recommended as it helps keep the vaginal area dry by not retaining heat or moisture. Avoid Tight Clothing: Loose-fitting clothes reduce heat and moisture buildup, lowering infection risks. Skip Douching: Douching and scented feminine products can disrupt the natural balance of bacteria in the vagina. Change Out of Wet Clothes: Promptly changing out of wet bathing suits or workout gear can prevent moisture accumulation. Good Bathroom Habits: Always wipe from front to back to avoid spreading bacteria. Manage Diabetes: Keeping blood sugar levels under control is essential for reducing yeast infections. Be Cautious with Antibiotics: Use antibiotics only when necessary, as they can kill beneficial bacteria that prevent yeast overgrowth. Diet and Hygiene: Consuming yogurt with active cultures can help maintain healthy bacteria levels, and using unscented, hypoallergenic soaps can prevent irritation. By prioritizing hygiene, ventilation, and healthy lifestyle choices, women can significantly reduce the risk of yeast infections, especially during the summer months. It’s essential to seek medical advice for proper diagnosis and treatment to avoid complications or resistant infections. With these proactive measures, women can enjoy the warmer weather comfortably and confidently. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Battling Knee Bursitis: Causes, Symptoms, And Treatment Options
Battling Knee Bursitis: Causes, Symptoms, And Treatment Options Knee bursitis, characterized by inflamed fluid-filled sacs near the knee joint known as bursae, can cause discomfort and limit mobility. Understanding its causes, symptoms, and treatment options is crucial for effective management and prevention. Causes and Symptoms: Knee bursitis often results from friction and irritation of the bursae, commonly occurring over the kneecap or on the inner side of the knee. Symptoms include warmth, tenderness, and swelling in the affected area, accompanied by pain during movement or at rest. Risk Factors and Prevention: Prolonged kneeling, certain sports activities, obesity, and underlying medical conditions like osteoarthritis increase the risk of developing knee bursitis. Preventive measures include wearing kneepads, taking regular breaks during activities involving prolonged kneeling, and maintaining a healthy weight. Diagnosis: Healthcare professionals diagnose knee bursitis through a combination of medical history evaluation, physical examination, and imaging tests such as X-rays, MRI scans, and ultrasounds. Aspiration, a procedure to drain bursa fluid, may be performed to test for infection or gout. Treatment Options: Treatment aims to alleviate symptoms and may include medications like antibiotics for bacterial infections, corticosteroid injections to reduce inflammation, and physical therapy to strengthen muscles and improve flexibility. In severe cases or when conservative measures fail, needle aspirations and surgical procedures such as bursa removal may be recommended. Understanding knee bursitis and its management options is essential for individuals experiencing symptoms or at risk of developing the condition. Prompt diagnosis and appropriate treatment can help alleviate discomfort, improve mobility, and prevent recurrence, allowing individuals to maintain an active and healthy lifestyle. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Urinary Tract Infections During Pregnancy: What Expecting Mothers Need To Know

Urinary Tract Infections During Pregnancy: What Expecting Mothers Need To Know Urinary tract infections (UTIs) pose a common health concern for women, with susceptibility increasing during pivotal life stages such as pregnancy. Understanding the causes, symptoms, and effective management strategies is crucial for maintaining overall well-being. UTIs typically occur when bacteria, most common being Escherichia coli (E. coli), infiltrate the urinary tract, sometimes involving different parts of the urinary system: the bladder, urethra, ureters, and kidneys. The close proximity of the urethra to the anus facilitates bacterial entry. Additional factors contributing to UTIs include weakened immunity, hormonal fluctuations, certain contraceptives, menopause, urinary tract anomalies, inadvertent sex, and hygiene habits. Recognizing UTI symptoms is paramount for timely intervention. These may manifest as a frequent urge to urinate, accompanied by a burning sensation, cloudy or foul-smelling urine, lower abdominal discomfort, and occasionally, hematuria. More severe cases may entail fever, chills, and fatigue, indicative of kidney involvement. While home remedies can mitigate mild UTI symptoms, seeking medical evaluation is imperative for persistent or worsening conditions. Diagnostic urine analysis aids in identifying the causative bacteria and tailoring appropriate antibiotic therapy. Completing the prescribed antibiotic course is essential to eradicate the infection fully and prevent recurrence. Pregnancy amplifies susceptibility to UTIs due to physiological changes. The expanding uterus exerts pressure on the bladder, impeding complete voiding, while hormonal shifts, notably elevated progesterone levels, predispose to ureteral relaxation and stasis. Left untreated, UTIs during pregnancy may escalate to kidney infections, jeopardizing maternal and fetal health. Symptoms of UTIs during pregnancy may mirror normal physiological changes, necessitating vigilance and consultation with healthcare providers. Routine prenatal urine tests facilitate early detection of UTI. Antibiotics deemed safe for pregnancy are prescribed promptly upon confirmation of UTIs, emphasizing the importance of adherence to the treatment regimen. Preventive measures play a pivotal role in mitigating UTI risk. Adequate hydration, prompt voiding post-intercourse and meticulous perineal hygiene reduce bacterial proliferation. Avoiding irritants like harsh soaps and bubble baths further fortifies preventive efforts. In conclusion, UTIs are a prevalent concern for women, particularly during pregnancy. Empowering individuals with knowledge about UTI triggers, symptoms, and management strategies is imperative for promoting women’s health. By embracing proactive measures and seeking timely medical intervention, women can effectively navigate UTIs, ensuring optimal well-being for themselves and their unborn children. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Managing Postpartum Hemorrhage For Maternal Well-Being
Managing Postpartum Hemorrhage For Maternal Well-Being Postpartum hemorrhage (PPH), characterized by severe vaginal bleeding after childbirth, poses a serious threat, potentially leading to fatal consequences. Recognizing symptoms like dizziness, faintness, and blurred vision is crucial, as early detection and prompt intervention are key to a successful recovery. Whether occurring immediately after delivery or up to 12 weeks postpartum, PPH demands immediate attention. Postpartum hemorrhage is defined by a blood loss exceeding 500 ml after normal childbirth, and 1000 ml after caesarean delivery. The two types, primary (within 24 hours) and secondary (24 hours to 12 weeks postpartum), require distinctive approaches. Causes and Risk Factors: The four Ts—tone, trauma, tissue, and thrombin are the major 4 determinants of PPH. Uterine atony, inadequate contractions post-delivery, accounts for 80% of cases. Contributing factors include retained placental tissue, uterine trauma, and blood clotting disorders. Symptoms: Persistent excessive bleeding, accompanied by symptoms like dizziness, increased heart rate, and abdominal pain, signals potential PPH. Timely reporting of symptoms is crucial, even if they manifest days or weeks postpartum. Diagnosis:General condition of patients, complete haemogram, Visual examinations, blood tests, and ultrasound scans aid in diagnosis. Monitoring the vital signs plays a vital role. Treatment of PPH: PPH, the medical emergency, demands urgent treatment. Approaches include uterine massage, medications to induce contractions, and, in severe cases, surgical interventions like laparotomy or hysterectomy. Prevention: Identifying high-risk individuals, addressing placental problems, and administering preventive medications during delivery contribute to reducing PPH risks. Adequate prenatal care, iron intake, and awareness of risk factors aid prevention. In conclusion, understanding, recognizing, and addressing postpartum hemorrhage are vital for maternal well-being. Timely intervention and a comprehensive approach contribute to positive outcomes, ensuring a healthy and safe postpartum period for both mother and child. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Osteomalacia: Causes, Symptoms, And Treatment
Osteomalacia: Causes, Symptoms, And Treatment Osteomalacia, often referred to as “soft bones,” is a metabolic bone disorder characterized by insufficient mineralization, leading to weakened and softened bones. Unlike osteoporosis, which involves the deterioration of existing bone, osteomalacia is a failure in the bone-building process. This condition primarily affects adults, whereas a similar deficiency in children leads to rickets. Bone is a living tissue undergoing continuous turnover. The outer shell, or cortex, is hard, while the inner structure, or matrix, resembles a honeycomb. Layers of calcium and phosphorus fortify this structure. Vitamin D is crucial in regulating these minerals, aiding calcium absorption from food to strengthen bones. Causes of Osteomalacia Osteomalacia stems from deficiencies in vitamin D, calcium, or phosphorus. Common factors contributing to vitamin D deficiency include: Poor intake of vitamin D-rich Inadequate exposure to Conditions like celiac disease, certain cancers, and surgeries impacting nutrient Kidney and liver disorders can affect vitamin D Drugs for epilepsy, such as phenytoin and phenobarbital, can interfere with vitamin D Insufficient dietary phosphate can also People at higher risk include those who are frail, wear clothing that covers most of their skin, have dark skin, or are pregnant or breastfeeding. Symptoms of Osteomalacia Bone pain in the legs, groin, upper thighs, knees, and sometimes the feet, especially when standing or walking. Muscle pain especially after exercise, affecting the thighs, shoulders, and trunk, leading to difficulties in climbing stairs, rising from chairs, and, in severe cases, getting out of Bones break more easily, particularly in the hips, lower back, and A waddling gait due to muscle weakness and bone Muscle cramps and pins and needles in the hands and feet due to low calcium Diagnosis: Blood tests X-rays Bone biopsy Treatment: Treatment involves addressing underlying causes and supplementing with vitamin D and calcium. Prevention: Spend time outdoors to facilitate natural vitamin D Consume foods rich in vitamin D, such as fatty fish and fortified dairy Consider vitamin D supplements if deficient or at Incorporate calcium sources like dairy, green leafy vegetables, and fortified Engage in weight-bearing activities to support bone Maintain a healthy weight, limit alcohol and caffeine, quit smoking, and have regular medical monitoring. Early diagnosis and proper treatment are crucial for managing symptoms and preventing complications. Seeking medical help from an experienced orthopedist ensures timely care, appropriate diagnosis, and effective treatment of osteomalacia. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Preeclampsia: Navigating Pregnancy Challenges

Preeclampsia: Navigating Pregnancy Challenges Preeclampsia, a condition exclusive to pregnancy, unfolds after the 20th week and is marked by high blood pressure and protein in the urine. Risk Factors: First-time moms face History of gestational hypertension or preeclampsia increases risk of ecclampsis Family history plays a crucial Multiple pregnancies elevate Extreme maternal age amplifies the Pre-existing conditions like high blood pressure or kidney disease heighten the Obesity, indicated by a BMI of 30 or more, is a significant Recognizing Symptoms: Preeclampsia may emerge without Blood pressure exceeding 130/90 mm Hg — confirmed on two occasions — signals a Mild preeclampsia shows signs like high blood pressure, water retention, and protein in the urine. Severe cases manifest with headaches, blurred vision, upper abdominal pain, and decreased urine output. Other indicators include excess protein in urine, severe headaches, vision changes, and impaired liver function. Diagnosis and Monitoring: Routine blood pressure checks are pivotal during prenatal Urine, kidney, and blood-clotting tests provide additional Ultrasound and Doppler scans evaluate fetal growth and blood flow to the Treatment Approach: Timely delivery is crucial, especially near the due For milder cases, rest, dietary changes, and increased prenatal checkups are Severe cases may involve blood pressure medication, bed rest, and dietary Impact on Mothers: Untreated preeclampsia can lead to liver or renal Complications like eclampsia and HELLP syndrome pose life-threatening Impact on Babies: Insufficient blood flow to the placenta may result in low birth Early detection and proper prenatal care improve Causes: The origin is linked to placental dysfunction, affecting blood vessel Inadequate blood flow, vessel damage, immune system irregularities, and genetic factors Proactive Measures: Control salt Hydrate Adopt a balanced Prioritize rest and In conclusion, while preeclampsia lacks a definitive preventive method, proactive health measures and vigilant prenatal care can mitigate risks. Early detection remains paramount for safeguarding both maternal and fetal well-being. Seeking medical guidance and adhering to prescribed interventions are imperative for navigating the challenges posed by preeclampsia. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Essential Newborn Care: A Guide For New Parents

Essential Newborn Care: A Guide For New Parents Welcoming a newborn into the world is a time of immense joy and responsibility. The first 28 days, known as the neonatal period, are crucial for laying the foundation for your baby’s long- term health and development. Whether you’re a first-time parent or seasoned caretaker, here are key aspects of newborn care to ensure your baby’s well-being and comfort. Feeding Essentials Feeding is a primary concern for new parents. It is advised to exclusively breastfeed for six months. it right is important for your baby’s health. Breastfeeding provides numerous benefits, including essential nutrients and bonding opportunities. Start feeding within the first hour of birth, let your baby nurse frequently to establish a strong milk supply, and ensure a proper latch to prevent discomfort. Avoid bottle feeding as it has high risk of infection and lactation failure. Holding and Bonding Handling a newborn can be daunting. Always wash/sanitize your hands before holding your baby, and provide support to their head and neck. Avoid shaking or bouncing your baby, as their fragile bodies require gentle handling. Bonding with your baby through physical contact is crucial. Spend time cradling, caressing, and talking to your baby, keeping stimulation gentle to foster emotional development. Diapering and Bathing Diapering is a frequent task; expect about ten changes a day. Have all necessary supplies ready, such as clean diapers. Treat diaper rash with ointment and warm baths. Daily body bath is recommended. Limit head bath to 2 times a week. Use soft, unscented products and keep the bathing environment clean and comfortable. Sleeping and Health Newborns sleep 16-18 hours a day, often in 2-4 hour stretches. Create a calm sleeping environment and establish a bedtime routine to help your baby adjust. Ensure safe sleep practices, like placing your baby on their back to sleep. Regular check-ups and vaccinations are vital for monitoring your baby’s growth and protecting them from diseases. Umbilical Cord Care The umbilical cord stump needs careful attention until it falls off naturally, typically within 1-3 weeks. Keep it clean and dry, and avoid moisture by folding the diaper below the stump. Watch for signs of infection, such as redness or swelling, and consult your pediatrician if needed. First bath is recommended after the umbilical stump falls. Essential Supplies Prepare your home with essential newborn items, including a crib, crib mattress, burp cloths, receiving blankets, bibs, and diaper rash cream. Each item supports various aspects of baby care, from feeding to hygiene. Navigating the early days with a newborn can be challenging, but with these tips and a supportive network, you’ll provide the best care for your baby. Embrace this beautiful journey with patience and love, and don’t hesitate to reach out to your pediatrician for guidance. Your dedication will help your baby thrive and grow into a healthy, happy child. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Internal And External Fixation In Fracture Treatment
Internal And External Fixation In Fracture Treatment Fracture treatment often necessitates repositioning and stabilizing bone fragments to ensure proper healing. Internal and external fixations are common methods used by orthopedic surgeons to achieve this, employing various implants to maintain bone alignment and promote recovery. These techniques not only reduce hospital stays but also help patients regain function more quickly and decrease the risk of improper bone healing. Internal Fixation: Techniques and Benefits Internal fixation involves using implants such as plates, screws, nails, and wires to hold broken bone fragments together. These implants are made from durable materials like stainless steel, titanium, cobalt, and chrome, which are compatible with the body and rarely cause allergic reactions. Plates: Plates function as internal splints, attached to the bone with screws to hold broken pieces together. Depending on the fracture’s nature, plates may remain in place permanently or be removed after healing. Screws: Screws are the most frequently used implant for internal fixation due to their versatility. They come in various sizes to match different bones and fracture types. Screws can be used alone or in conjunction with other implants such as plates and rods. After the bone heals, screws can either be left in place or removed. Nails or Rods: For long bone fractures, nails or rods are often inserted through the bones. Bolts at each end of the rod prevent the fracture from shortening or rotating, ensuring the rod stays in place until the bone This method is commonly used for femur and tibia fractures, with rods and screws typically left in place after healing. Wires/Pins: Wires or pins are used to hold small bone fragments together, particularly in the hands or feet. They are often employed in conjunction with other fixation methods but can be used alone for certain small bone fractures. Depending on the fracture, wires may be removed after a certain period or left in place permanently. External Fixation: Temporary and Permanent Solutions External fixators serve as stabilizing frames that hold broken bones in place using metal pins or screws inserted into the bone through the skin and muscle. These pins and screws are connected to a bar outside the skin, providing external support. External fixators are commonly used as temporary solutions, particularly for patients with multiple injuries who are not yet ready for long surgical procedures. They offer good stability until the patient is healthy enough for definitive surgery. In some cases, external fixators are used as the primary method to stabilize bones until complete healing. Internal and external fixations are essential techniques in fracture management, providing stability and promoting efficient healing. Understanding these methods and their applications helps in making informed decisions about fracture treatment, ensuring the best possible outcomes for patients. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…

