Types Of Pain
Types Of Pain Pain can be classified into two primary types: neuropathic pain and nociceptive pain. These types of pain are distinguished by their causes and how they affect the body. Neuropathic Pain Neuropathic pain originates from the nerves or nervous system. It often results from nerve damage or diseases like sciatica or conditions caused by a bulging or slipped disc. Neuropathic pain can be persistent, sometimes lasting longer than nociceptive pain, and is often described as sharp, burning, or tingling. Nociceptive Pain Nociceptive pain is more common and arises from damage to the body’s tissues, such as muscles, bones, or organs. This pain is often caused by injuries like bruises, sprains, fractures, or conditions such as arthritis. Nociceptive pain can vary in intensity, from dull, throbbing aches to sharp, sudden cramps. It can be either chronic or recurring, depending on the cause. Pain Mechanism Pain is triggered when receptor neurons in tissues like the skin, muscles, joints, bones, or organs detect harmful stimuli. These stimuli can be mechanical (pressure), chemical (irritants), or thermal (temperature). The receptors transmit signals to the brain, which interprets them as pain. For example, if something hot presses against your skin, the nociceptive receptors sense both heat and mechanical pressure, resulting in pain. Treatment Options Treatment for both types of pain focuses on relieving symptoms and treating the root cause. Options include: Over-the-counter pain relievers – to reduce pain and inflammation Therapeutic massage – to ease muscle tension and promote circulation Physical therapy – to strengthen muscles and improve flexibility Occupational therapy – to help with daily activities Pain-relieving injections – to reduce inflammation and manage pain Laser or energy therapies – for targeted pain relief Managing Chronic Pain Acute pain from injuries usually resolves within weeks. However, chronic pain, such as that caused by arthritis or degenerative conditions, can last longer and may require ongoing treatment. Managing nociceptive pain often involves a combination of therapies to effectively reduce symptoms and improve quality of life. Recent Posts Types Of Pain Types Of Pain Pain can be classified into two primary types: neuropathic pain and nociceptive… Pilon Fracture Pilon Fracture A pilon fracture is a specific break in the lower shinbone (tibia) near… Coping With Morning Sickness: A Guide For Expectant Mothers Coping With Morning Sickness: A Guide For Expectant Mothers Morning sickness is one of the… Finding Relief From Chronic Pain: When To Seek Help Finding Relief From Chronic Pain: When To Seek Help Living with chronic pain can feel…
Pilon Fracture

Pilon Fracture A pilon fracture is a specific break in the lower shinbone (tibia) near the ankle joint, often involving multiple bone fragments. In some cases, the smaller fibula bone also breaks. These fractures are typically complex fractures and require specialized treatment due to their complexity. Causes of Pilon Fractures Pilon fractures often result from high-energy impacts. Falls from a height, such as from ladders or during skiing, are common causes. Motor vehicle and pedestrian accidents can also transmit significant force to the lower leg, leading to fractures. In rare cases, severe sports injuries, like forceful landings or collisions, may cause pilon fractures. Symptoms of Pilon Fractures Symptoms include severe pain localized to the ankle, significant swelling, and bruising. Deformity of the ankle joint may be noticeable, and bearing weight on the injured leg is typically impossible. In some cases, nerve damage may cause numbness or tingling in the foot. Diagnosing Pilon Fractures Doctors diagnose pilon fractures through a combination of methods. A physical examination assesses pain, swelling, and deformity. X-rays provide a clear view of the broken bone fragments, while CT scans are used in complex cases for detailed imaging of the fracture pattern. Treatment Options Treatment depends on the severity of the fracture. Surgical intervention, such as Open Reduction and Internal Fixation (ORIF), is common for severe fractures, using plates, screws, or rods to stabilize the bone. Non-surgical options include immobilization with a cast or boot, pain management with medications, and physical therapy to restore strength and mobility. Recovery Process Recovery from a pilon fracture can take months. Immobilization in a cast or boot is required for several weeks, followed by physical therapy to rebuild strength and flexibility. Pain management is essential during the initial healing phase and therapy. Potential Complications Complications may include infections, improper bone healing (nonunion or malunion), arthritis due to cartilage damage, or chronic pain in the ankle joint. Preventing Pilon Fractures Prevention involves caution on uneven surfaces, wearing proper footwear, and engaging in balance exercises like yoga. Protective gear during sports and gradual skill development can also reduce risk. Awareness and preventive measures help avoid such severe injuries. Recent Posts Pilon Fracture Coping With Morning Sickness: A Guide For Expectant Mothers Morning sickness is one of the… Coping With Morning Sickness: A Guide For Expectant Mothers Coping With Morning Sickness: A Guide For Expectant Mothers Morning sickness is one of the… Finding Relief From Chronic Pain: When To Seek Help Finding Relief From Chronic Pain: When To Seek Help Living with chronic pain can feel… Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment The shoulder joint, a ball-and-socket structure formed by…
Coping With Morning Sickness: A Guide For Expectant Mothers

Coping With Morning Sickness: A Guide For Expectant Mothers Morning sickness is one of the most common and challenging symptoms of early pregnancy. Despite its name, it can occur at any time of the day, not just in the morning. Affecting up to 80% of pregnant women, this condition usually starts around the sixth week of pregnancy and typically eases by 12 to 14 weeks. Morning sickness refers to the nausea and vomiting experienced during the first trimester of pregnancy. It is believed to be linked to rising levels of pregnancy hormones, particularly human chorionic gonadotropin (hCG) and oestrogen. For most women, it is a sign of healthy hormonal changes. However, in some cases, nausea and vomiting become severe—a condition known as Hyperemesis Gravidarum (HG). This requires medical attention as it can lead to dehydration and nutrient deficiencies. The exact cause is not fully understood, but several factors may contribute: Hormonal Changes: Higher levels of hCG and estrogen are associated with nausea. Heightened Sense of Smell: An increased sensitivity to smells may act as a protective mechanism to avoid harmful foods. Family history of morning sickness. Tendency to experience migraines or motion sickness. Presence of Helicobacter pylori, a bacteria linked to stomach ulcers. Carrying multiples, such as twins or triplets, due to elevated hormone levels. Tips for Managing Morning Sickness Keep dry snacks, like crackers, by your bedside and eat a few before getting out of bed. Get up slowly to avoid sudden movements that can worsen nausea. Avoid letting your stomach become too empty or too full, as both can trigger nausea. Focus on light, bland foods. Drink fluids between meals instead of with meals to reduce the feeling of fullness. Avoid rich, spicy, or heavily flavored dishes that may worsen symptoms. Cold or room-temperature meals, such as salads or cold meats, can be less nauseating than hot, aromatic meals. Ginger is a natural remedy for nausea. You can try ginger tea, ginger ale, or ginger tablets. Lemon can also help. Strong odors from cooking, garbage, coffee, or petrol are common triggers. Choose a protein-rich, low-glycemic snack before sleep to help maintain stable blood sugar levels overnight. Options include yoghurt, milk, or a slice of wholegrain bread. Snack Ideas to Keep Nausea at Bay Keep simple, easy-to-digest foods on hand to snack on during the day: Plain crackers, rice cakes, or corn thins. Fresh fruit. Toast or pikelets. Plain cereal or rice. Small portions of pasta. Morning sickness can feel overwhelming, but remember that it’s temporary and often a sign of a healthy pregnancy. Reach out to your healthcare provider if you’re struggling to keep food or fluids down. Recent Posts Coping With Morning Sickness: A Guide For Expectant Mothers Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment The shoulder joint, a ball-and-socket structure formed by… Finding Relief From Chronic Pain: When To Seek Help Finding Relief From Chronic Pain: When To Seek Help Living with chronic pain can feel… Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment The shoulder joint, a ball-and-socket structure formed by… Understanding Kidney Stones During Pregnancy Understanding Kidney Stones During Pregnancy Pregnancy can bring about many health changes, and one potential…
Finding Relief From Chronic Pain: When To Seek Help
Finding Relief From Chronic Pain: When To Seek Help Living with chronic pain can feel isolating and overwhelming. It impacts every facet of your life, from your professional responsibilities to your personal relationships. If you’re grappling with persistent pain, it’s essential to seek help at a pain relief center. Here are the four main reasons when you should seek help: You’re Struggling with Daily Activities Chronic pain can rob you of the joy in activities you once cherished. If you find it increasingly challenging to work, exercise, or engage socially, it’s a clear sign that you should consider pain management solutions. Don’t let discomfort diminish your quality of life. Reaching out for help can pave the way for a more fulfilling existence. Over-the-Counter Treatments Aren’t Working Many individuals begin their pain management journey with over-the-counter remedies, such as pain relievers and anti-inflammatory drugs. While these options may provide temporary relief for some, they often fall short for those suffering from chronic pain. If these treatments haven’t alleviated your discomfort, it may be time to explore more comprehensive alternatives available at a specialized pain relief center. Side Effects Are Impacting Your Life If you are relying on prescription pain medications, you might be dealing with unwanted side effects such as drowsiness, constipation, or nausea. Although these effects can often be managed, they can still hinder your ability to enjoy daily life. If you’re finding it hard to cope with these side effects, discussing your situation with your healthcare provider can help you find better solutions tailored to your needs. Pain Disrupts Your Sleep Chronic pain frequently disrupts sleep patterns, making it difficult to enjoy restful nights. If you’re waking up in discomfort or struggling to fall asleep, this sleep deprivation can lead to fatigue, irritability, and difficulty concentrating. It’s vital to address these sleep issues by consulting your doctor about pain management strategies that can help restore your nightly rest. Don’t let chronic pain dictate your life. Seeking treatment early on can significantly improve your well-being and allow you to reclaim the activities you love. Remember, taking that first step towards relief is a courageous move towards a brighter, more enjoyable future. Recent Posts Finding Relief From Chronic Pain: When To Seek Help Finding Relief From Chronic Pain: When To Seek Help Living with chronic pain can feel… Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment The shoulder joint, a ball-and-socket structure formed by… Understanding Kidney Stones During Pregnancy Understanding Kidney Stones During Pregnancy Pregnancy can bring about many health changes, and one potential… Sciatica: Causes, Symptoms, And Treatment Options Sciatica: Causes, Symptoms, And Treatment Options The sciatic nerve is the longest and largest nerve…
Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment
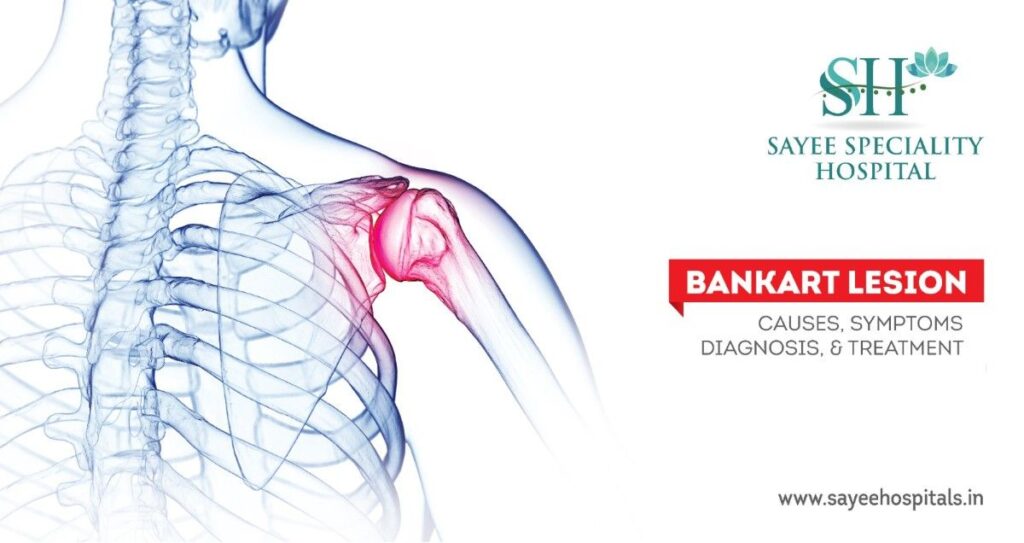
Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment The shoulder joint, a ball-and-socket structure formed by the humerus and scapula, is vital for arm movement. When dislocated, particularly through an injury, it can lead to a Bankart lesion, a tear in the labrum—a ring of cartilage that stabilizes the shoulder joint. This condition results in pain, swelling, and stiffness. Symptoms of Bankart Lesion Individuals with a Bankart lesion may experience: Intense shoulder pain that intensifies over time. Weakness and instability in the shoulder during daily activities. Limited range of motion. Other symptoms may include swelling, numbness, bruising, and audible popping sounds. Causes of Bankart Lesion While Bankart lesions are often seen in athletes, they can affect anyone. Common causes include: Overuse of the shoulder joint. Sports collisions or falls. Car accidents. Incidents like slipping on sidewalks or falls during activities like gymnastics or skiing. Loose ligaments that predispose individuals to dislocation. Diagnosis of Bankart Lesion A thorough physical examination is essential, but imaging tests like MRI or X-rays are typically required to confirm the diagnosis. An MRI provides detailed images of the soft tissues and glenoid cavity, assisting the orthopedic surgeon in determining the appropriate treatment. Treatment Options Treatment varies based on age, activity level, symptoms and severity. Non-surgical methods often include rest, bracing, slings, and physiotherapy focused on restoring strength and mobility. If these methods fail, surgical interventions such as shoulder arthroscopy or open surgery may be necessary. Post-Surgery Recovery Patients may need to wear a sling for 3-4 weeks and commence physiotherapy shortly after surgery. Returning to sports is typically possible after six months, depending on individual recovery and severity of the initial injury. Recent Posts Finding Relief From Chronic Pain: When To Seek Help Finding Relief From Chronic Pain: When To Seek Help Living with chronic pain can feel… Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment The shoulder joint, a ball-and-socket structure formed by… Understanding Kidney Stones During Pregnancy Understanding Kidney Stones During Pregnancy Pregnancy can bring about many health changes, and one potential… Sciatica: Causes, Symptoms, And Treatment Options Sciatica: Causes, Symptoms, And Treatment Options The sciatic nerve is the longest and largest nerve…
Understanding Kidney Stones During Pregnancy

Understanding Kidney Stones During Pregnancy Pregnancy can bring about many health changes, and one potential issue that may arise is the development of kidney stones. These solid masses form when calcium combines with other substances in urine, leading to blockages in the urinary tract. Understanding the symptoms, treatment options, and ways to manage kidney stones during pregnancy is essential for both mothers and their healthcare providers. Recognizing Symptoms Women who develop kidney stones while pregnant may experience several discomforting symptoms: Pain during urination: This sharp pain can be severe enough to make urination extremely difficult. Nausea and vomiting: The discomfort from kidney stones and the pressure on the kidneys can lead to feelings of sickness. Blood in urine: While seeing blood in urine can be alarming, it may occur without being linked to serious complications. Back or abdominal pain: This pain might indicate urinary retention, where a blockage causes urine to build up in the kidneys, potentially leading to a condition known as hydronephrosis, especially in later stages of pregnancy. Risks of Miscarriage While kidney stones do not directly cause miscarriage, untreated stones can lead to complications like urinary tract infections, which may increase miscarriage risk. This possibility underscores the importance of addressing kidney stone issues promptly. Treatment Options Treatment for kidney stones varies based on their size and the individual circumstances of the pregnant woman. Some options include: Medications: Doctors may prescribe muscle relaxants to ease ureter blockage. Sound wave therapy: This non-invasive method uses vibrations to break down stones, though it can be painful. Surgery: In cases where other methods fail, minimally invasive surgery might be necessary. Scope procedures: This involves using a scope via urethra to break up stones and may require anesthesia. Pain Relief Strategies For those experiencing pain from kidney stones, consider these strategies while waiting for treatment: Drinking plenty of water can help dilute urine and assist in passing stones. Evaluate calcium supplements: Reducing calcium intake may lower the risk of developing more stones. This has to be done only after your doctor’s consultation. In summary, if you suspect kidney stones, seek medical advice quickly to minimize risks and ensure a healthy pregnancy. Recent Posts Finding Relief From Chronic Pain: When To Seek Help Finding Relief From Chronic Pain: When To Seek Help Living with chronic pain can feel… Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment The shoulder joint, a ball-and-socket structure formed by… Understanding Kidney Stones During Pregnancy Understanding Kidney Stones During Pregnancy Pregnancy can bring about many health changes, and one potential… Sciatica: Causes, Symptoms, And Treatment Options Sciatica: Causes, Symptoms, And Treatment Options The sciatic nerve is the longest and largest nerve…
Sciatica: Causes, Symptoms, And Treatment Options

Sciatica: Causes, Symptoms, And Treatment Options The sciatic nerve is the longest and largest nerve in the human body, originating in the lower back and extending to the feet. It plays a critical role in movement, sensation, and reflexes. Movement: Controls muscles in the buttocks, legs, knees, and lower legs. Sensation: Enables feeling in the back of the thighs, lower legs, and soles of the feet. Reflexes: Helps maintain lower-body reflexes. Disruption of the sciatic nerve can lead to pain and mobility challenges, highlighting its vital role in daily activities like walking and standing. Causes and Locations of Sciatic Pain Sciatica refers to pain caused by irritation or compression of the sciatic nerve. Common causes include: Herniated Disc: A damaged spinal disc pressing on nerve roots. Spinal Stenosis: Narrowing of the spinal canal, affecting nerve roots. Piriformis Syndrome: Spasms or tightness in the piriformis muscle pressing on the nerve. Injury: Direct trauma to the lower back or buttocks. Pain locations depend on where the nerve is affected: Lower Back: The starting point of discomfort. Buttocks: Pain often radiates here from the lower back. Legs and Feet: Pain may extend down one or both legs, reaching the feet in severe cases. Sciatic pain can feel sharp, burning, or electric, and it may be accompanied by tingling, numbness, or muscle weakness. Treatment Options for Sciatica A pain management doctor specializes in diagnosing and treating conditions like sciatica. Treatments include: Medications: Pain relievers, anti-inflammatory drugs, and muscle relaxants. Physical Therapy: Strengthening exercises and stretches to alleviate pressure on the nerve. Injections: Steroid injections or nerve blocks to reduce inflammation and pain. Lifestyle Changes: Weight management, improved posture, and regular exercise. In most cases, sciatica is treatable without surgery. For severe cases, options like spinal cord stimulation or surgical procedures may be considered. Pain physicians tailor treatment plans to individual needs, helping patients find relief and regain mobility. Recent Posts Finding Relief From Chronic Pain: When To Seek Help Finding Relief From… Bankart Lesion: Causes, Symptoms, Diagnosis, And Treatment Bankart Lesion: Causes,… Understanding Kidney Stones During Pregnancy Understanding Kidney Stones…
Avascular Necrosis: Causes, Symptoms, And Treatments
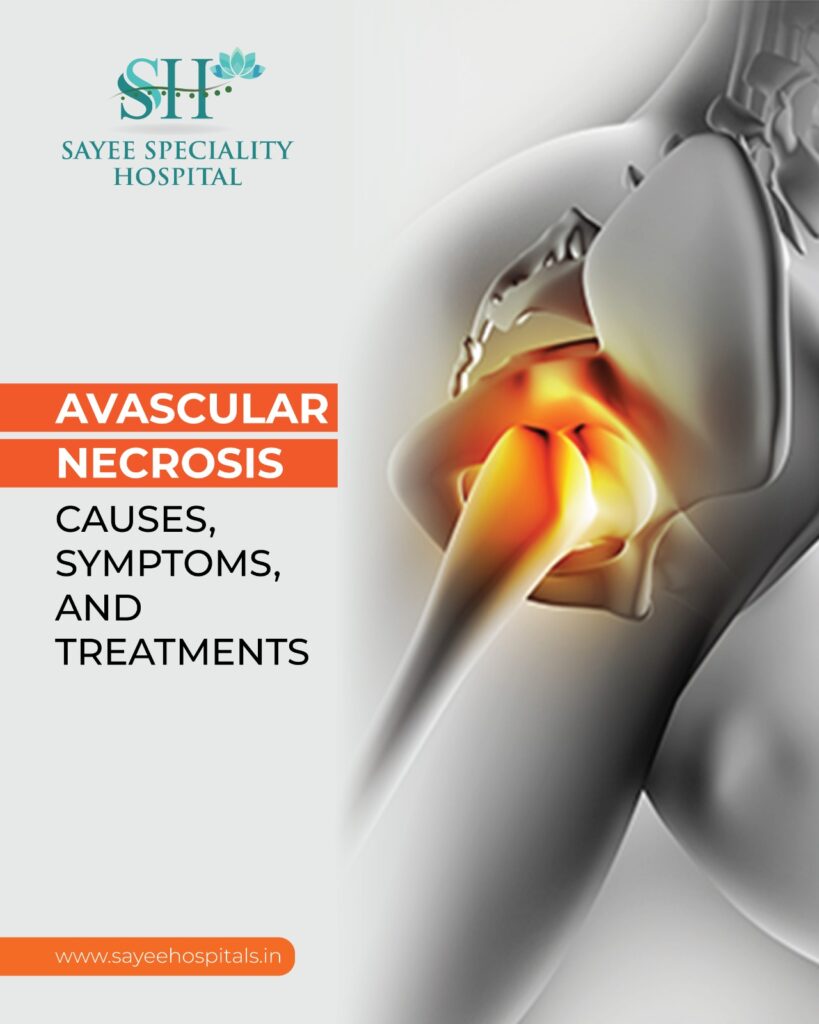
Avascular Necrosis: Causes, Symptoms, And Treatments Avascular necrosis (AVN), or osteonecrosis, is a painful condition that occurs when the blood supply to bone tissue is reduced or completely cut off, leading to tissue death. While it primarily affects the hip joint, AVN can also impact the knees, shoulders, and ankles. If untreated, this condition can lead to bone collapse. AVN typically affects individuals between the ages of 20 and 50 and is caused by a range of factors. Injuries like fractures or dislocations, long-term use of steroid medications, and excessive alcohol consumption are common contributors. Certain medical treatments, such as radiation therapy or organ transplants, as well as chronic conditions like diabetes, lupus, and sickle cell anemia, can also increase the risk. Inflammation, blood clots, effect of covid-19 or damage to arteries that supply blood to the bone are additional factors that may lead to AVN. Early stages of AVN often present no noticeable symptoms, which can delay diagnosis. Over time, joint pain, particularly under pressure, may develop. Symptoms can progress to stiffness, limping, reduced range of motion, and difficulty performing daily activities like walking or climbing stairs. If the joint collapses, excruciating pain may occur, making movement nearly impossible. Diagnosis begins with a physical examination to assess tenderness and joint mobility. Imaging tests like X-rays, MRI, or CT scans help detect the condition, while bone scans can pinpoint areas of reduced blood supply. Treatment for AVN depends on factors such as the stage of the disease, the affected area, and the patient’s age. Early-stage AVN can often be managed with non-surgical options like medications, crutches to reduce weight on the affected joint, and exercises to maintain mobility. Medications include NSAIDs for pain relief, blood thinners for clot-related AVN, and cholesterol-lowering drugs to prevent blockages. Surgical options may be necessary for advanced cases. These include core decompression, osteotomy, bone grafts, total joint replacement, and vascularized bone grafts. Surgeons may also use electrical stimulation during procedures to promote bone regeneration. Preventive measures can reduce the risk of AVN. Limiting alcohol intake, avoiding smoking, using steroids responsibly, and managing cholesterol levels are effective strategies. Early detection and proactive treatment are key to minimizing complications and preserving joint function. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Pediatric Arrhythmias: Understanding And Managing Abnormal Heart Rhythms

Pediatric Arrhythmias: Understanding And Managing Abnormal Heart Rhythms Pediatric arrhythmias are irregular heart rhythms that can disrupt a child’s normal heart function, leading to potential health complications if left untreated. These conditions can range from mild to severe, affecting the heart’s ability to pump blood and oxygen effectively. Early diagnosis and timely treatment are essential to ensuring better outcomes for children with arrhythmias. Types of Pediatric Arrhythmias Different types of arrhythmias impact children in distinct ways. Tachycardia, characterized by a rapid heart rate, may require medications or other interventions. Bradycardia, where the heart beats slower than normal, can pose issues if it affects overall health. Premature atrial contractions (PACs) and premature ventricular contractions (PVCs) are extra heartbeats in the upper and lower chambers, respectively, and often require careful observation to determine their significance. Recognizing Symptoms Recognizing the symptoms of pediatric arrhythmias is crucial. Signs include an unusually fast or slow heart rate, dizziness, fainting, chest pain, difficulty breathing, fatigue, and anxiety. These symptoms can vary depending on the severity of the condition, but early detection can significantly improve the effectiveness of treatment. Causes of Pediatric Arrhythmias The causes of pediatric arrhythmias are diverse. Genetic predispositions, congenital heart defects, and certain medications, such as those used for asthma or ADHD, are common contributing factors. Additionally, viral infections and electrolyte imbalances can disrupt the heart’s normal rhythm, further emphasizing the need for thorough assessment. Treatment Options Treatment for pediatric arrhythmias depends on the type and severity of the condition. Medications like beta-blockers and calcium channel blockers help regulate heart rate and rhythm. Ablation therapy, a minimally invasive procedure, targets abnormal heart tissue to restore normal function. For severe cases, pacemakers or implantable cardioverter-defibrillators (ICDs) are used to maintain or correct heart rhythms. Other advanced options, such as cardioversion or maze surgery, address more complex cases effectively. Pediatric arrhythmias, though concerning, can be managed successfully with timely care and appropriate treatment. Recognizing symptoms, understanding causes, and tailoring treatment to the child’s specific needs are key steps in ensuring improved heart health and a better quality of life. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…
Understanding Menstrual Disorders: Types, Causes, And Impacts

Understanding Menstrual Disorders: Types, Causes, And Impacts Menstrual disorders are common conditions that can affect women’s physical and emotional health. They encompass a range of issues, from irregular cycles to excessive bleeding and severe pain. Understanding the types and causes of these disorders can help in managing the conditions effectively. Types of Menstrual Disorders Dysmenorrhea (Painful Cramps): Dysmenorrhea involves intense cramping in the lower abdomen that may spread to the lower back and thighs. Primary Dysmenorrhea: Caused by uterine contractions during menstruation, often severe during heavy bleeding. Secondary Dysmenorrhea: Linked to medical conditions like endometriosis or uterine fibroids. Menorrhagia (Heavy Bleeding): Menorrhagia refers to prolonged or heavy menstrual bleeding. It involves soaking more than five sanitary pads daily or experiencing bleeding for more than seven days. Often accompanied by clotting and painful cramps, it may result from hormonal imbalances, fibroids, or other structural issues. Amenorrhea (Absence of Menstruation): Amenorrhea is categorized into two types: Primary Amenorrhea: The absence of menstruation by age 16, often due to delayed puberty or genetic factors. Secondary Amenorrhea: Periods stop for at least three months after previously being regular, often caused by pregnancy, stress, hormonal imbalances to name a few. Oligomenorrhea and Hypomenorrhea: Oligomenorrhea refers to infrequent periods occurring more than 35 days apart, often seen in adolescents. Hypomenorrhea is characterized by light menstrual flow, which is common in early puberty or before menopause. Premenstrual Syndrome (PMS): PMS includes physical, emotional, and behavioral symptoms that occur a week before menstruation. It commonly affects women aged late 20s to early 40s. Causes of Menstrual Disorders Hormonal Imbalances: Variations in estrogen and progesterone levels. Medical Conditions: Endometriosis, polycystic ovarian syndrome (PCOS), thyroid dysfunction, or uterine abnormalities. Lifestyle Factors: Excessive exercise, stress, or significant weight changes. Genetic Conditions: Bleeding disorders like von Willebrand disease. Structural Issues: Uterine fibroids, polyps, or scarring. Menstrual disorders, while common, can significantly impact a woman’s quality of life. Adopting a healthy lifestyle can reduce menstrual discomfort. Regular exercise, minimizing alcohol and smoking, and managing stress contribute to better menstrual health. During periods, adequate rest, warm beverages, heating pads, and balanced meals can help alleviate discomfort. Timely medical attention and self-care ensure better management of menstrual health challenges. Recent Posts The Silent Emergency: Understanding Ovarian Torsion THE SILENT EMERGENCY: UNDERSTANDING OVARIAN TORSION Most people have never heard of ovarian torsion. And… Influenza In Children: Causes, Symptoms, And Prevention Influenza In Children: Causes, Symptoms, And Prevention Influenza, commonly known as the flu, is a… Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment Sacroiliac Joint Pain: Causes, Diagnosis, And Treatment The sacroiliac (SI) joint plays a crucial role… Safe And Effective Exercises During Pregnancy Safe And Effective Exercises During Pregnancy Staying active throughout pregnancy offers a range of benefits…

